See Explanation
[]
Gastroenterology
intestinal disorders
celiac disease
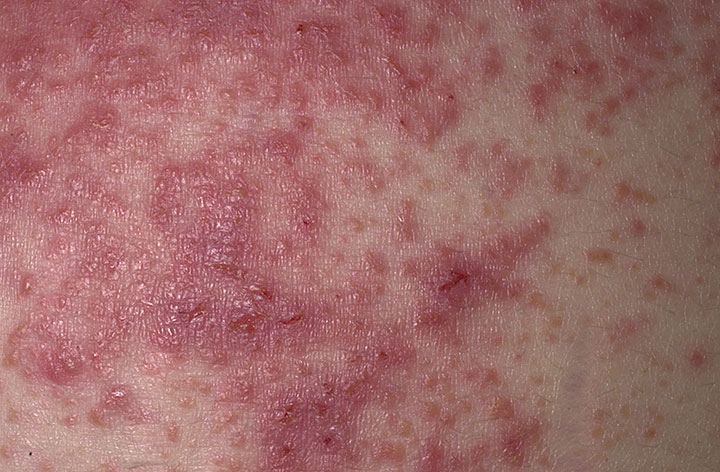
A 55-year-old woman with a 5-year history of celiac disease, diagnosed after chronic malabsorption, presents to the emergency department with a 2-week history of acutely worsening abdominal pain, severe fatigue, and persistent low-grade fevers (up to 38.5°C). She reports significant unintentional weight loss of 7 kg over the past 3 months and has recently noticed dark, tarry stools. Her long-standing celiac disease has been challenging to manage, with periods of dietary non-compliance despite repeated counseling. On examination, she appears cachectic and pale. Her temperature is 38.8°C, blood pressure is 95/60 mm Hg, and pulse is 98/min. Abdominal examination reveals diffuse tenderness, most pronounced in the periumbilical region, without rebound or guarding. Bowel sounds are diminished. Rectal examination confirms melena. Given this presentation, what is the most appropriate next diagnostic step and the critical immediate management consideration?
| Lab Parameter | Value | Reference Range |
|---|---|---|
| Hemoglobin | 85 g/L | 125-170 g/L |
| Mean corpuscular volume | 70 fL | 80-100 fL |
| Platelets | 280 x 10^9/L | 130-380 x 10^9/L |
| Leukocytes | 11.2 x 10^9/L | 3.5-10.5 x 10^9/L |
| Blood urea nitrogen | 4 mmol/L | 2.5-8.0 mmol/L |
| Creatinine | 70 µmol/L | 70-120 µmol/L |
| Albumin | 31 g/L | 35-50 g/L |
| Erythrocyte sedimentation rate | 87 mm/h | <15 mm/h |
| C-reactive protein | 75 mg/L | <5 mg/L |
| Serum Ferritin | 8 µg/L | 20-300 µg/L |
Edit question